Motuz ’24 Celebrates Health After 12 Surgeries and Complications from Cleft Lip and Palate
At 18-years-old, Arcadia University biology major Mychajla Motuz ’24 has undergone 12 facial reconstruction surgeries to fix her cleft lip and palate, which were complicated by a childhood infection that nearly killed her, and a blood disease.

Motuz’s first surgery was at three months old when she had lip surgery, as well as her frenulum under her tongue cut to fix her tongue tie and tubes put in her ears. That’s when doctors discovered she had Lupus anticoagulant factor, an immunoglobulin that causes her blood to not clot. In order to have surgeries to reconstruct her palate and face, Motuz has to undergo testing before each surgery to ensure her blood clots in the correct amount of time.
Throughout childhood, Motuz has undergone surgery every few years to help correct issues as she grows, including grafting a section of hip bone to her upper jaw to cover a hole between her nose and front teeth.
“I could blow air through it and have it come out my nose—it was my childhood party trick,” jokes Motuz. “That was probably one of the hardest surgeries to recover from because not only was my face healing, but my hip too.”
The other difficult surgery Motuz recalls was supposed to be one of the simplest: cutting down her tonsils and adenoids. After two surgeries to have her tonsils and adenoids removed, this time doctors planned to cauterize the tissue after the organs were cut down to try and keep them from regenerating. However, the equipment had been imported from China and contaminated, which caused Motuz to nearly die from an infection that led to septic shock.
“It was just a few days before my sixth birthday,” Motuz recalls. “I remember waking up and the left side of my body was red from the infection. It’s the only surgery I’ve had where anything really went wrong, and so we switched to [Children’s Hospital of Philadelphia] after that happened.”
Her most recent surgery was July 2019, which reconstructed her nose.
“My doctor told me that how my nose was angled probably kept me from breaking it in high school when I played soccer,” Motuz said with a smile, recounting how an opponent hit her in the face with the ball and then her head. “Because of the way my anatomy was already misshaped, it just kept bending instead of snapping.”
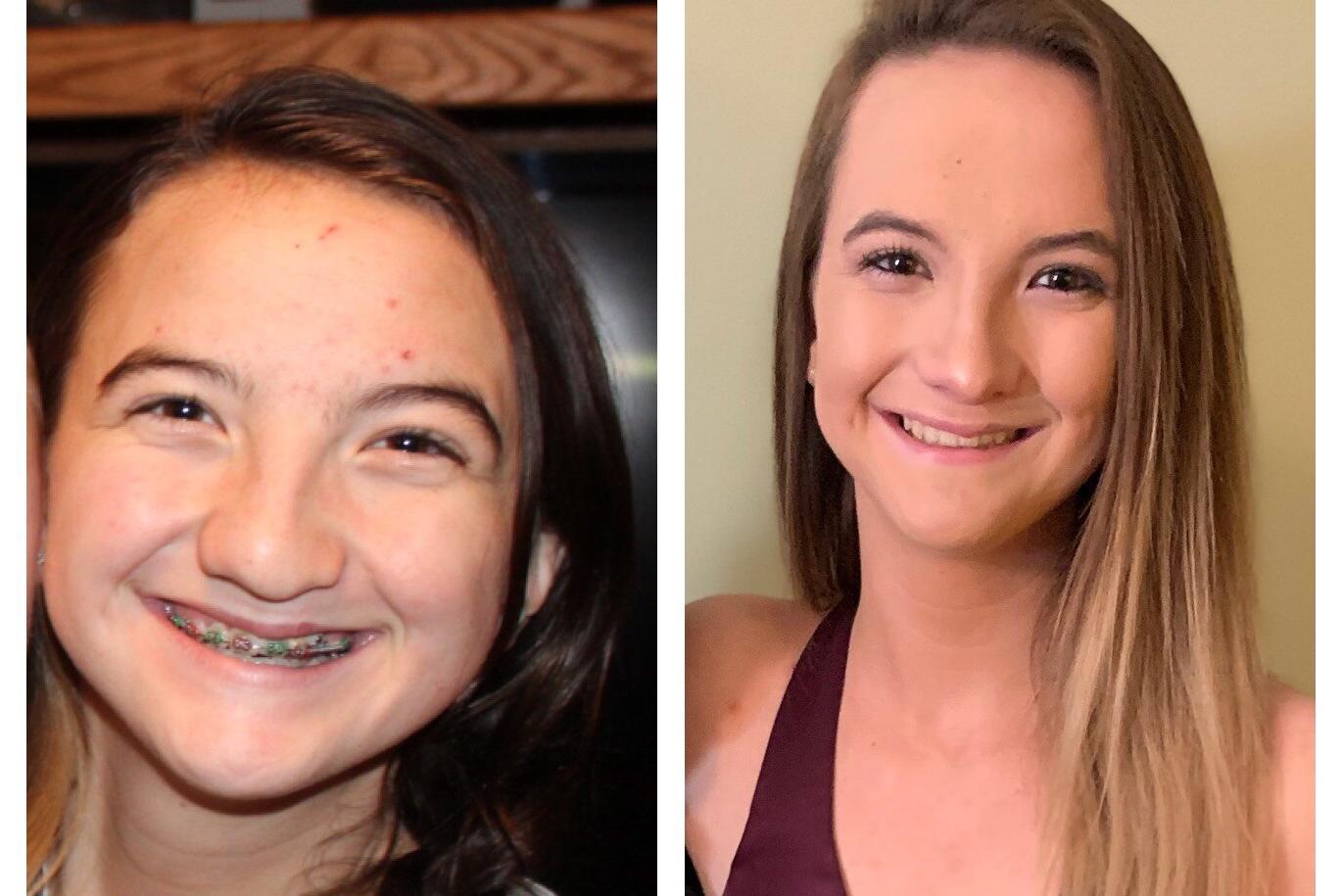
Motuz’s before and after photos following double jaw and nose surgeries.
In elementary school, Motuz was given the nickname “smile,” coming from her sunny disposition toward life. Through the consultations, surgeries, complications, and recoveries, she’s smiled (or did the best she could).
“I could either smile, or be crushed by it,” said Motuz. “I think anyone who’s in my situation would do the same, because these aren’t elective procedures. I have to have these surgeries.”
Motuz credits her mother, whom she calls her personal super hero, for also keeping her going through all of it: “My mom is my biggest supporter and she has gotten me through every doctor appointment and every surgery.”
Approximately 1,600 children are born each year with a cleft palate, which is when the tissue in the roof of the mouth doesn’t meet and causes a hole between the mouth and nasal cavity. This genetic condition requires several surgeries throughout childhood to correct, and sometimes requires double-jaw surgery, where the top and bottom jaw is broken on each side and then reset with steel plates.
Motuz is currently writing a book about her experience with double-jaw surgery, which she had in December 2018. At 16-years-old, she’s one of only a few young adults to have the surgery, which usually occurs after age 20. However, to help Motuz breathe better and relieve a pinched nerve near her left ear, doctors felt it was necessary to do the surgery.
“I couldn’t find any information about having the surgery as a kid,” said Motuz, who uses her personal experiences and information from her doctor for her book. She also catalogued her recovery through photos. “I want other children and their families to have the information and to know what to expect.”
Now that Motuz is finally done with her cleft palate surgeries, she’s using the experience to inform her career path. On the pre-med track at Arcadia, she plans on being a cleft palate surgeon, with research interests in nerve and tissue regeneration in order to help children born with cleft lips and palates.
“I want to create some type of injection for the lip to help stimulate the tissue to grow naturally in order to cut down the number of invasive surgeries children with cleft experience,” said Motuz. “The most common and most noticeable is cleft lip. I want to make it easier for children growing up so they have more muscle control and reduced scarring.”


